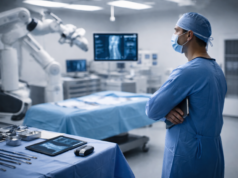
Every operating room runs on rhythm. Speech-based technology often sounds like it belongs in an OR environment. Hands-free interaction can remove a step, keep people in position, and limit unnecessary movement. That promise holds up in some rooms. In others, the noise, timing, and pace make voice recognition harder to rely on. Whether these systems help or get in the way usually comes down to how well they align with the habits of the room.
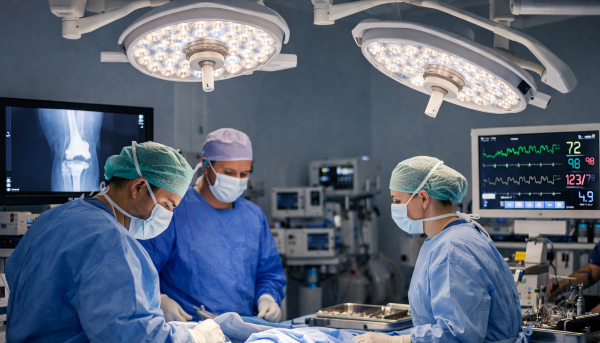
Why voice control keeps coming up in the OR
Voice control keeps resurfacing because it aligns with sterile technique. You are constantly navigating what you need to do and what you are allowed to touch. AORN guidance reinforces the importance of maintaining sterility throughout a procedure and responding quickly when contamination becomes a concern.
That pressure influences how teams move and communicate during a case. Tools that respect that balance blend in quickly. Tools that interrupt it are noticed just as fast. In practice, these systems rarely work well on their own. They work best alongside other touch-free options rather than trying to handle everything through spoken commands. Surgeons are more receptive when these features stay out of the way and do not demand extra attention.
Where voice control actually saves time
Voice control saves time during routine actions that interrupt a case when they require extra coordination. For example, adjusting overhead lighting. Without voice control, the surgeon asks, an assistant moves into position, the adjustment is made, and the surgeon confirms it is correct. With voice control, that exchange happens in one step, allowing the case to proceed without interruption.
The same applies during time-out and before closing. When voice control is used to acknowledge items already spoken aloud during these required safety pauses, teams move through confirmations without stopping to manage equipment or documentation. Thus, time is saved by removing unnecessary steps.
Where problems show up in the OR
Problems appear fast after missed commands or unpredictable responses. A single misfire can break concentration and send you back to a slower workaround. Over time, consistency matters more than raw speed. Uneven performance across cases weakens confidence, even if the system works well under ideal conditions.
That impact extends beyond the person giving the command. As more technology enters the room, cognitive demands spread. Nursing staff absorb much of that pressure, especially when added operational demands pull attention away during already busy cases. Time saved for one person can quietly turn into extra strain for someone else.
What effective voice control looks like in an orthopaedic OR
The real test happens on an ordinary day, not during a demo. Teams trust systems that behave the same way across cases. Reliable behavior helps cases continue without added mental strain.
Tools designed for a narrow purpose integrate more easily. Systems that try to manage too much at once draw attention at the wrong moments and lose credibility. Voice-based interfaces also require training and coordination. FDA guidance on computer-assisted surgical systems emphasizes clear expectations and appropriate training, which applies just as much to voice interaction as it does to hardware.
Deciding whether voice control is worth it for your team
The question is less about capability and more about impact. A system earns its place when it reduces delays without adding work for someone else in the room. When it causes hesitation or shifts the workload unevenly, the strain is felt almost immediately. In that context, voice-based technology is about finding the right fit for your OR.
Sources
AORN Guideline in Focus: Sterile Technique in the OR
Computer-Assisted Surgical Systems
Using Gesture and Speech to Control Surgical Lighting Systems: Mixed Methods Study