Orthopaedic training has moved well beyond cadaver labs and early-morning case reviews. For surgeons in practice, whether overseeing residents or refining skills in subspecialty procedures, simulation-based tools are becoming more integrated into education, credentialing, and even preoperative planning. These platforms now offer measurable value across the training spectrum — from novice to attending — providing detailed feedback and opportunities to close skill gaps without stepping into an OR.
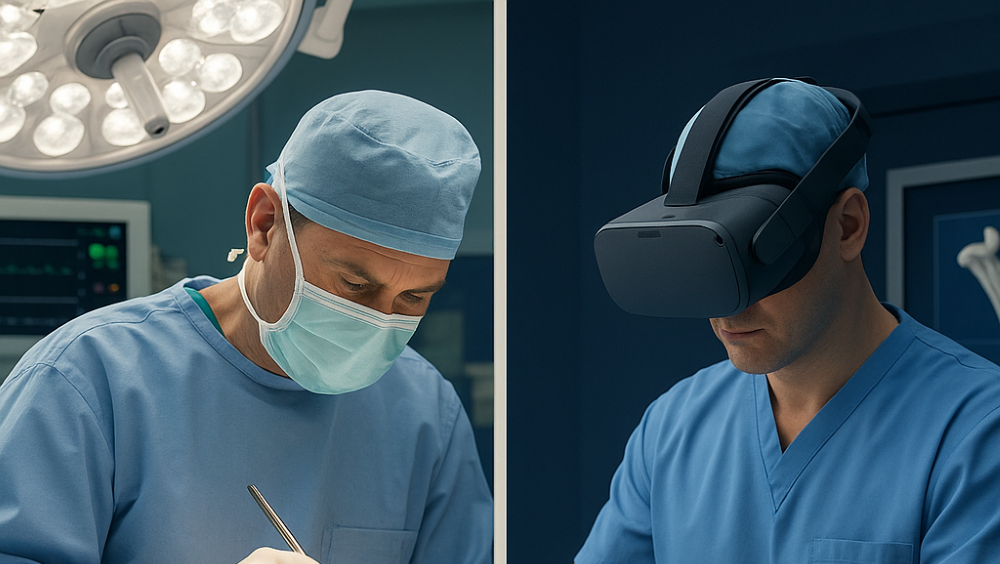
Why VR is gaining ground in orthopaedics
Virtual reality has matured beyond novelty. Modern simulation systems provide more than visual walkthroughs. They combine anatomic realism with tactile feedback and procedural precision, creating environments that closely replicate real surgical scenarios.
Surgeons using platforms such as Osso VR, Preclinic-Sim, PrecisionOS, and ImmersiveTouch can rehearse procedures with layered anatomy, responsive force feedback, and complication modules that reflect real-case variability. These tools are now being used not only for resident education but also for continuing surgical refinement, especially in procedures where volume has dropped or techniques have evolved.
Rather than waiting for rare cases to appear, you can now rehearse them directly. Revision total hip arthroplasty and complex fracture reconstructions are accessible on demand. For those in subspecialty roles, this technology supports preparation for unfamiliar implants or changes in surgical approach.
AI is turning feedback into actionable insight
Artificial intelligence now handles much of the performance analysis inside simulation systems. These tools track metrics well beyond time and completion: screw trajectory, soft-tissue retraction force, exposure angle, efficiency of movement, and adherence to stepwise protocols are all captured and scored.
Studies show that AI scoring correlates with human faculty evaluations over 90 percent of the time. The advantage is consistency and scale. Whether you’re monitoring a resident or auditing your own simulation session, the data is clear, repeatable, and actionable. More advanced systems also flag trends across cases — identifying, for instance, repeated over-tensioning or persistent angle deviation in tunnel placement.
This supports more targeted coaching. Whether you’re mentoring a junior attending or adjusting your own muscle memory, these insights allow for faster correction and more deliberate refinement.
Simulation isn’t just for skill building
Modern simulators also model decision-making under pressure. Advanced systems now introduce intraoperative challenges that force users to choose alternate fixation strategies, respond to unexpected anatomy, or modify plans mid-case.
In practice, these scenarios can sharpen your response to complications, particularly in revision surgery or unfamiliar trauma patterns. The simulators track not only what decision is made, but how long it takes, whether it follows best practices, and how the case unfolds afterward.
For attendings teaching in the OR, this is a way to preview and evaluate how a resident or fellow responds under stress. For practicing surgeons, it offers a structured space to rehearse cognitive branching before stepping into high-risk cases.
Know where simulation still falls short
While simulation has improved dramatically, limitations persist. No simulator yet replicates the full variability of live tissue. Soft-tissue behavior, bleeding, suction control, and true surgical exposure challenges remain difficult to model. In the OR, many variables still shift unpredictably, including patient anatomy and assistant performance.
Simulator environments also lack the team-based complexity of surgery. You’re not dealing with real scrub techs or anesthesia input that regularly shape how a case unfolds.
This doesn’t reduce simulation’s value, but it frames its role. Use these tools to refine your own technique, prepare for infrequent procedures, and evaluate trainee readiness. Just don’t assume they fully replace the need for OR-based decision-making experience.
Competency models are catching up
Residency and fellowship programs are moving toward performance-based progression. For current surgeons, this affects how you evaluate and credential trainees — and how you track your own development in low-frequency procedures.
Simulation supports this model by producing data that goes beyond logbooks. Objective skill metrics can now supplement or even replace case counts for credentialing in some programs. A surgeon returning to practice after leave or expanding into a new procedural domain may find that simulation-based proficiency tracking accelerates their re-entry.
In practical terms, this reframes the focus from exposure to performance. Instead of relying on whether someone has seen a case, you can now ask whether they’ve demonstrated proficiency in executing it correctly. This reduces risk, improves outcomes, and makes remediation more structured.
A useful tool, when applied deliberately
Simulation-based training now offers orthopaedic surgeons real opportunities (beyond initial education) to improve technique and assess readiness. Whether you’re maintaining rare procedural skills or adapting to new surgical technologies, high-fidelity simulation and AI-driven feedback can support safer, smarter practice.
Used correctly, these tools create an environment where preparation is deliberate, feedback is specific, and growth is measurable. They won’t replace live surgery or human mentoring. But in a specialty where technical mastery defines outcomes, simulation now plays a supporting role worth taking seriously.
Sources
Mastering Orthopedic Surgery through Simulation
Virtual Reality Surgery Training: The Future of Precision Medical Education