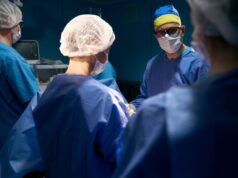
A single-institution series of 142 cementless TKAs in patients older than 75 years reported excellent mid-term survivorship, with 99.3 percent aseptic and 98.6 percent all-cause implant survivorship and no progressive radiolucencies or subsidence at latest follow-up.
Similarly, a 2025 propensity-matched study comparing cementless tibial fixation to cemented tibial fixation in primary TKA found slower improvement in patient-reported outcomes over the first three to six months for cementless, yet no meaningful differences by twelve months in PROs, satisfaction, range of motion, complications, readmissions, or reoperations. The authors recommend counseling patients about a potentially slower early recovery with cementless tibial components.
While these results suggest cementless knees can perform well in older adults, hip data highlights a different set of concerns.
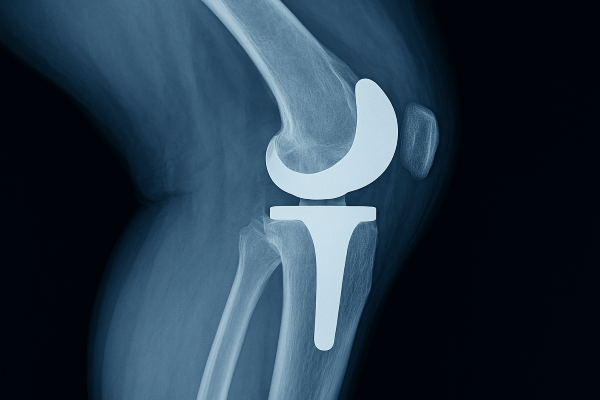
Why cement still has defenders in the hip
A recent Journal of Arthroplasty study compared survivorship, revision reasons, and PROMs between cementless and cemented stems in patients aged 70 years or older, reflecting renewed scrutiny of traditional age-based guidelines. Yet despite the shift toward cementless fixation in U.S. practice, registry and long-term study data point to fracture risk in older populations.
This concern is supported by long-term evidence. A 20-year study of more than 14,000 primary THAs found that cemented fixation reduced fracture risk by about 30 percent in women. In addition, registry data from more than 280,000 patients older than 65 years showed cementless stems, age above 80 years, and female sex were all linked with increased fracture risk. As a result, some surgeons to recommend cemented stems for patients older than 75 years, particularly women and those with balance or cognitive concerns.
Study context and interpretation: While these registry and cohort studies provide valuable insight, they carry inherent limitations such as selection bias, evolving implant designs, and variability in surgical technique. These factors may influence fracture risk independent of fixation method. Still, the consistency of the findings across large datasets strengthens the case for cement in higher-risk patients.
International practice differences: It is also worth noting that practice patterns vary widely across regions. In the U.S., cementless fixation has become dominant, partly due to training patterns and confidence in modern porous designs. In contrast, European surgeons continue to favor cemented stems in older adults, citing lower fracture rates and extensive registry support. Fixation choice reflects not only evidence but also the influence of training patterns and healthcare systems.
How surgeons are moving the decision from age to mechanics
In a recent interview, RB Jones, MD, explained that he no longer relies on an age cutoff when deciding on cementless knees. Instead, he places greater emphasis on intraoperative factors such as implant stability and preparation. He estimated that about 90 percent of his current knee replacements are cementless when trialing shows sufficient stability, noting that he has performed roughly 1,000 such procedures using modern porous designs. This approach reflects a broader shift in practice, where decisions are guided less by patient age and more by considerations such as trial stability, bone quality, anatomic fit, and operating room efficiency gained by avoiding cement curing time.
Putting it to work in your practice
If you are considering cementless fixation in an older adult with good bone and strong trial stability, the knee data above supports durability while also reminding you to set expectations about a slower early recovery curve. For hips, the evidence supports cemented stems for older patients at higher fracture risk, especially women. Therefore, even with modern cementless designs, this remains a critical consideration when planning primary THA in patients older than 75 years.
Key factors to guide fixation choice:
- Bone quality: Assess density and cortical thickness. Poor bone stock may favor cemented fixation.
- Intraoperative stability: Stable trialing supports cementless; instability suggests cement may be safer.
- Patient profile:
- Age: Over 75, particularly women, may face higher fracture risk with cementless hips.
- Comorbidities: Balance problems, cognitive decline, or frailty increase fracture risk and may favor cement.
- Functional status: More active older patients with good bone may benefit from cementless durability.
- OR efficiency: Cementless fixation avoids cement curing time and may shorten operative workflow.
- Patient counseling: Inform knee patients that cementless fixation may mean slower recovery in the first 3–6 months, but outcomes equalize by one year.
Bottom line: Let fixation choices follow intraoperative stability and bone quality, but weigh fracture risk and survivorship data heavily when age and comorbidities raise concern.
Disclaimer: This article is for educational purposes only and not intended as medical advice. Fixation decisions should be based on each patient’s clinical profile, surgeon judgment, and current guidelines.
Sources
Cementless Total Knee Arthroplasty in Patients Older Than 75 Years
Should all patients aged 75 years or older receive cemented femoral components for primary THA?
What’s the right indication for cement versus cementless implants?