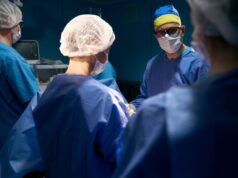
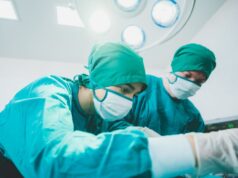
Every January, orthopaedic clinics hear variations of the same question: “Does cold weather make surgery riskier?” Patients report stiffer joints, more pain, and slower movement after a sedentary December, and naturally wonder if that should affect surgical timing. It’s a common debate, but when you look at the real data, the answers are subtler than most people assume.

What the evidence actually says about cold weather and joint symptoms
Many people with arthritis or chronic joint pain do report increased discomfort in cold or changing weather, but the scientific picture isn’t straightforward. A systematic review of observational studies found that weather conditions (including temperature, humidity, and barometric pressure) do correlate with reported osteoarthritis pain in many patients, suggesting that joint pain can fluctuate with weather factors. However, the strength of that correlation varies and doesn’t imply structural worsening of the disease itself.
Another large European study tracked joint pain and local weather (temperature, humidity, pressure) in older adults over time and found associations between certain weather variables and pain reports. However, it also emphasized that these relationships are complex and influenced by many factors.
At the same time, broader reviews of musculoskeletal symptoms suggest that while many patients feel weather impacts their pain, other data does not consistently link specific weather changes to measurable pain increases, highlighting that atmospheric conditions are only one piece of a much bigger clinical picture.
In other words: Cold or changing weather may be one of several contributors to symptom perception, but there’s no evidence that it worsens joint pathology in a way that increases surgical risk.
Does seasonal timing change surgical outcomes?
When it comes to actual surgery, the evidence is clear that season alone doesn’t change outcomes. For procedures such as total hip and knee arthroplasty, large outcome datasets show no meaningful seasonal differences in complication rates or infection risk. Patients see similar early functional outcomes regardless of when surgery is performed.
Instead, modifiable factors — patient comorbidities, optimization before surgery, rehabilitation planning, and fall risk mitigation — have far more impact than the season of the procedure itself.
What winter can influence
Although surgical outcomes don’t change with the calendar, winter conditions can affect recovery logistics for some patients:
- Icy walkways and slippery surfaces increase fall risk during early ambulation.
- Severe weather can disrupt physical therapy appointments or transportation.
- Peak respiratory illness season (e.g., influenza) may complicate recovery for vulnerable patients.
None of these are surgical risks per se, but they are real postoperative management considerations that warrant planning.
When winter can actually help
For many patients, winter timing is convenient — less travel, fewer social obligations, and more time at home can improve adherence to postoperative restrictions and physical therapy. Evidence shows that consistent engagement with rehab is one of the strongest predictors of functional improvement after joint replacement, season notwithstanding.
How to talk with your patients
The most useful counseling focuses on personal factors, not the calendar. A patient’s overall readiness, support systems, home safety (especially for winter footing), and rehabilitation environment matter far more than outdoor temperatures. Helping patients understand that symptom fluctuation with weather is common, but not dangerous, can reduce unnecessary delays in care.
Bottom line for winter scheduling
Cold weather may influence how patients feel before surgery, but it does not compromise orthopaedic surgical outcomes when proper clinical pathways are followed. With thoughtful planning around recovery logistics, winter procedures can be safe and predictable, just like those done in any other season.
Disclaimer: This article is for educational purposes only and not intended as medical advice. Decisions regarding surgical timing should be based on each patient’s clinical profile, surgeon judgment, and current evidence.
Sources
Prehabilitation and Rehabilitation for Major Joint Replacement
The Association of Season of Surgery and Patient Reported Outcomes following Total Hip Arthroplasty