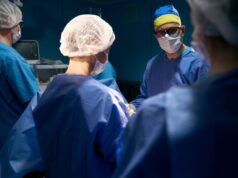
Exploring the promise and challenges of endoscopic fusion, where progress depends on standardization, validation, and measurable outcomes.
Missed the foundation of this series? Revisit Part 1: Balancing Innovation with Evidence to explore how data-driven decision-making shapes responsible adoption of minimally invasive techniques.
Endoscopic fusion has become one of the most ambitious and debated frontiers in minimally invasive spine surgery (MISS). Initially limited to decompression, endoscopy now extends into fusion procedures that aim to minimize tissue trauma and accelerate recovery. Yet as indications expand, the data supporting its broader use remain uneven.
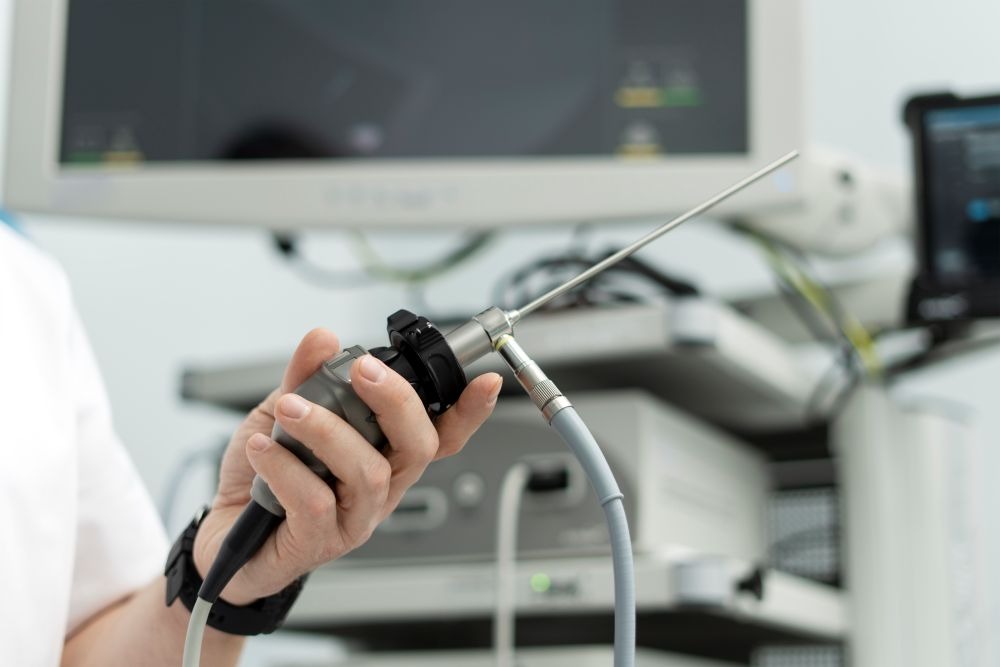
Expanding boundaries, uneven results
An analysis in the International Journal of Spine Surgery found that while outcomes for endoscopic decompression are consistently reliable, the evidence supporting endoscopic fusion is still developing. The review identified significant variability among techniques and noted that complication rates tend to cluster early in the learning curve. Researchers also emphasized that procedural standardization is lacking across centers, making comparisons difficult and replication even harder.
Surgeons agree that endoscopic fusion represents meaningful progress but caution that enthusiasm should be tempered by realism. A national survey published in the same journal found that most respondents see potential in endoscopic fusion but remain wary of its costs, prolonged learning curve, dependence on specialized technology, and limited long-term outcome data. These barriers contribute to slow skill acquisition and limit the volume of multicenter data available for large-scale analysis.
Measured gains and the need for validation
Despite these challenges, advances in instrumentation and visualization have improved procedural control. Smaller access corridors and integrated navigation now allow surgeons to perform complex tasks through minimal incisions. In experienced hands, and with careful patient selection, short-term results can rival those achieved with traditional open or tubular fusion.
However, these successes often come from high-volume centers or specialized teams with years of focused experience. Broader adoption has not yet translated into consistent outcomes across institutions. The field now faces a critical juncture: Validation must take priority over invention. Without rigorous trials and reproducible metrics, progress risks being fragmented by preference rather than guided by proof.
Setting standards for the future
A unified framework for defining success, both clinical and radiographic, could help bring structure to future research and guide patient expectations. Agreement on what constitutes fusion success, how to measure outcomes, and when to report complications would provide the clarity needed to move the field forward responsibly.
Endoscopic fusion is likely to strengthen as technology matures and as training becomes more structured. Yet the defining factor in its future will not be novelty but evidence. Data, not design, must determine its reach.
Part 3 of this series will explore how robotics and navigation may help close that evidence gap or widen it.
Sources
Endoscopic Spine Surgery: A French National Survey on Practices, Motivations, and Challenges