A closer look at how enthusiasm for minimally invasive techniques must be matched by data-driven decision-making and careful case selection.
Minimally invasive spine surgery (MISS) has reshaped modern spine care. What began as limited decompression has expanded to fusion and robotics. The discussion has shifted from proving MISS works to defining when it should be used.
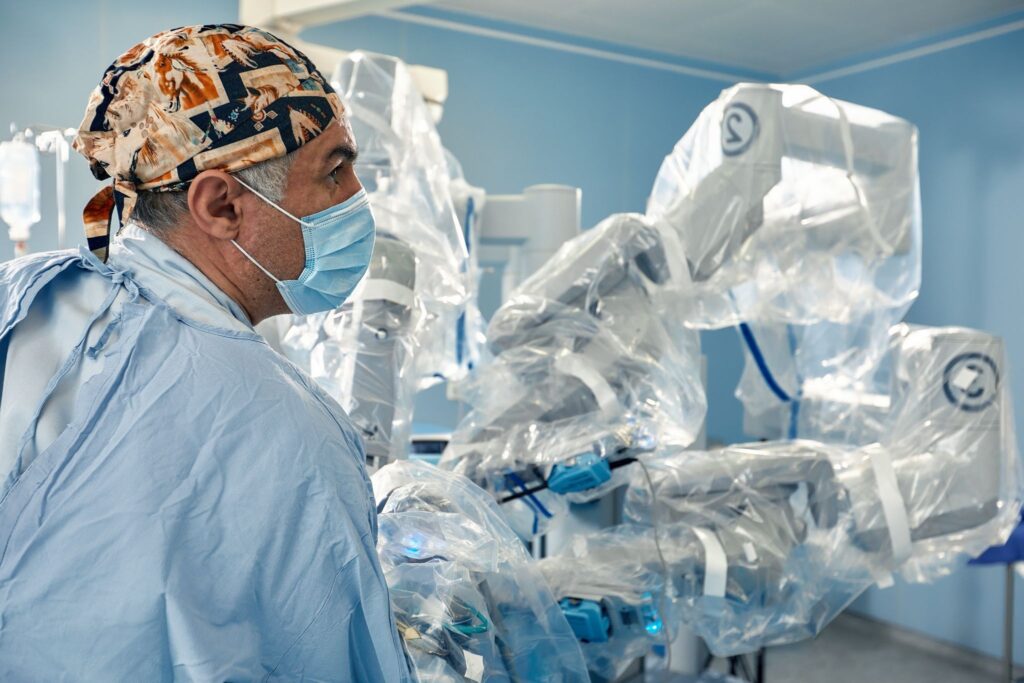
Expanding techniques and varying expertise
A recent review in The Spine Journal highlights how endoscopic lumbar procedures now encompass everything from microdiscectomy to fusion in carefully selected patients. While short-term outcomes often show reduced pain and quicker recovery, the success of these techniques remains closely tied to surgeon expertise and institutional resources. Inexperienced surgeons or low-volume centers may see wider variability in results.
A national survey published in the International Journal of Spine Surgery mirrors this. Enthusiasm for MISS continues to climb, yet adoption remains inconsistent due to training demands and limited access to advanced tools. Many surgeons view MISS as the future of spine care, but the data suggests that skill development and case selection remain the most important determinants of success.
Evidence strong for select procedures
There is strong evidence supporting minimally invasive transforaminal lumbar interbody fusion (MIS-TLIF), particularly for older adults with degenerative spondylolisthesis. These patients consistently experience lower blood loss, shorter hospital stays, and improved postoperative pain scores. However, the supporting literature weakens once procedures become more complex, such as multilevel fusions or cases requiring deformity correction. When endoscopic techniques replace traditional open exposure in these scenarios, long-term outcomes and fusion integrity remain uncertain.
A multicenter study involving more than 800 surgeons reported high reliability and reproducibility for MISS decompression but found limited proof of equivalence for fusion procedures. The growing role of robotics and navigation may change that, but early data remains mixed. A 2025 NASS Open Access review emphasized that the promise of these technologies depends on validated performance metrics, not perception or marketing claims.
Balancing innovation with restraint
MISS has clearly moved beyond its experimental origins; it has become an expectation in contemporary spine practice. Yet that expectation brings a new responsibility: ensuring that enthusiasm for innovation does not outpace the evidence guiding its use.
As minimally invasive options expand and technologies continue to advance, orthopaedic surgeons must weigh data over trends. The next phase in the evolution of MISS will rely less on proving capability and more on refining indication, using it when science, not sentiment, supports doing so.
This series will examine where the evidence currently stands and how surgeons can navigate the balance between innovation and restraint in modern spine care. Next week: Part 2 – Endoscopic Fusion and the Push for Standards.
Sources
Endoscopic Spine Surgery: A French National Survey on Practices, Motivations, and Challenges
The symbiosis of robotics, enabling technology and minimally invasive surgery